Why Patients with Kidney Disease are Missing Out on Hospice
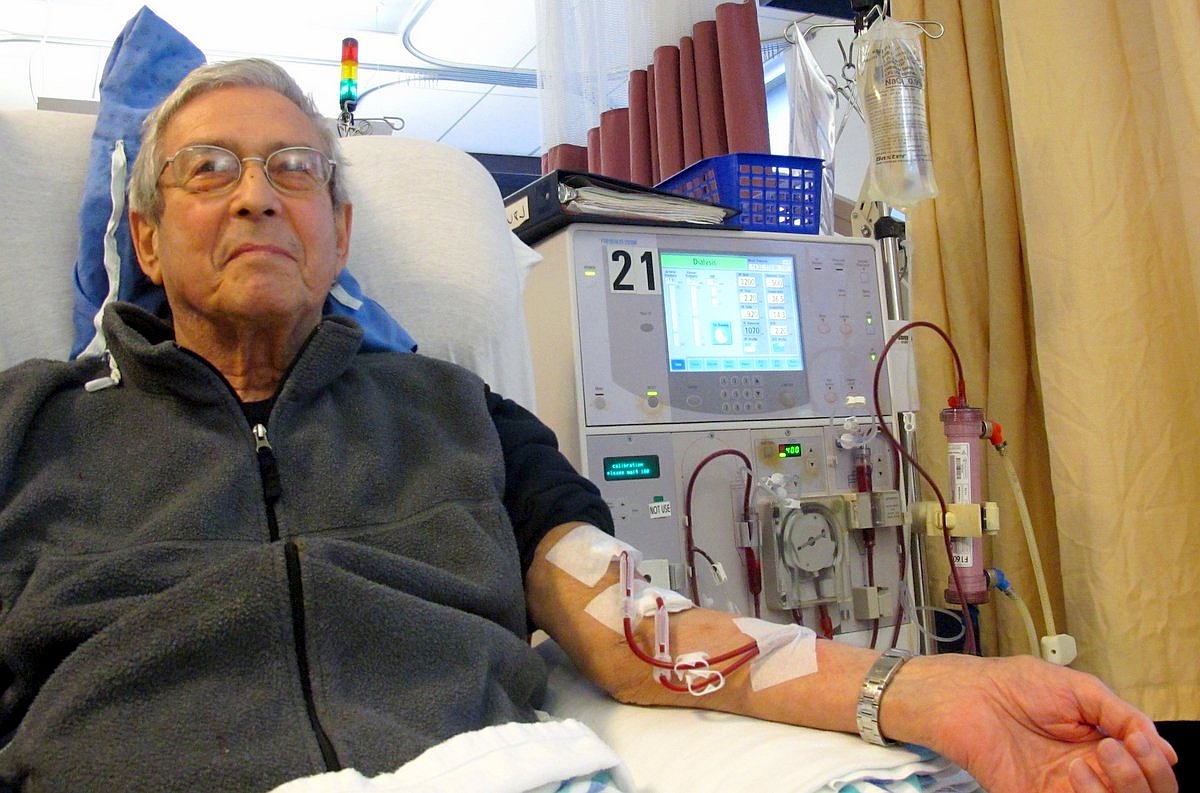
One of the most vexing – even heartbreaking – issues that seriously ill patients and their families face is the fact that referrals to hospice care often aren’t made until they are literally on their deathbeds. This is especially true for renal failure hospice patients. Renal failure is otherwise known as kidney disease.
According to the most recent Facts and Figures: Hospice Care in America report from the National Hospice and Palliative Care Organization, 48 percent of all Medicare decedents in 2016 received one day or more of hospice care and were enrolled in hospice at the time of death. The average length of service for Medicare patients enrolled in hospice in 2016 was 70 days. The median length of service was 23 days.
But a study reported April 30th, 2018, in JAMA Internal Medicine, found that only about 20 percent of Medicare patients with end-stage kidney disease were enrolled in hospice prior to death. And those who had used hospice were almost twice as likely to have very short stays (three days or fewer) compared to patients with other advanced serious illnesses.
Medicare Quandary
The problem? Current Medicare policy requires patients to stop receiving curative or disease-modifying therapies such as hemodialysis before they can be admitted to hospice.
“The fact is, most kidney disease patients pass within a week or so of ending dialysis treatments. As a result. they can only access hospice care for just a very short time,” said Dr. Walter George, Senior Vice President for Physician Education and Services at Crossroads Hospice & Palliative Care.
“That’s unfortunate, because hospice care specialists can do much to provide pain and symptom management and other support services for kidney disease patients as well as their families,” Dr. George said.
Additional hospice care can include nursing services, hospice aide services and psychosocial, spiritual and bereavement support. Still, to be eligible for hospice care, the patients need to be certified as likely to have six months or less to live if the disease runs its normal course.
There also may be countervailing circumstances. For example, a renal failure hospice patient who also has terminal lung cancer or end-stage heart failure or another comorbidity may still benefit from dialysis and continue to receive treatment.

Palliative Care Options
Nevertheless, patients with kidney disease should not overlook the benefits that palliative care can provide, Dr. George said. Patients who opt to continue receiving dialysis treatments can still turn to palliative care practitioners for pain management and other support services.
The basic goal of palliative care is to prevent and/or relieve pain and discomfort and to support the best possible quality of life for patients and their families, regardless of what stage their disease has reached and according to patients’ individual values and preferences.
Many people don’t realize that patients with end-stage kidney disease who are on dialysis often experience high levels of pain similar to what advanced cancer patients experience, Dr. George said. They also have a higher mortality rate.
“But palliative care practitioners, working with the patient’s primary physician, can help them devise goal-oriented treatment programs that allow them to alleviate pain and discomfort as much as possible while also help address end-of-life issues that may come up as their condition worsens over time,” he said.
The important thing is for patients and their primary doctors to be fully aware of their options and be willing to work with hospice and palliative care specialists to ensure that their personal choices are honored and that they have the opportunity to experience the best quality of life possible for as long as possible, Dr. George said.
To learn more about hospice eligibility for renal disease, give us a call at 1-888-564-3405.
Dialysis Patient Photo credit: Anna Frodesiak
If you found this information helpful, please share it with your network and community.
Copyright © 2018 Crossroads Hospice. All rights reserved.




