Body Positivity for Cancer & Palliative Care Patients

Embracing and loving one’s body, despite its imperfections or changing conditions, is the idea behind body positivity.
Once a fringe social movement that began in the 1960s as a way to challenge societal norms around body types, this concept has now become so mainstream that it’s the inspiration behind countless television commercials, ad campaigns, and social media hashtags.
“Body positivity is rooted in the belief that all of us should be comfortable in our skin,” says Joyce White, a Crossroads Hospice & Palliative Care social worker in Kansas City. “And it’s related back to our self-image.”
Because of its increased visibility in popular culture, body positivity – with how it has the potential to improve one’s emotional and physical well-being – is now even being incorporated in the ways that palliative care professionals like Joyce are interacting with cancer patients and others with chronic illnesses.
Through the use of various mindfulness tactics and exercises, and under the supervision of healthcare professionals, patients can achieve new levels of comfort and acceptance of their circumstances.
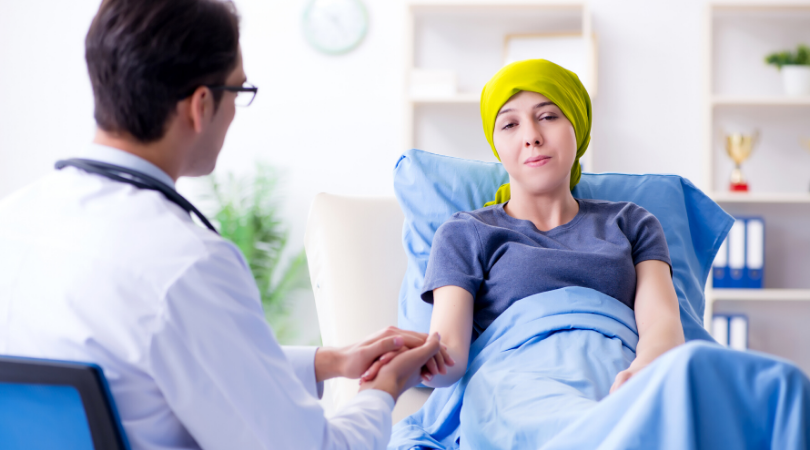
Learning to Accept the Physical Changes
Conditions like hair loss, limb amputation, weight loss, or severe skin rashes are all common side effects of various cancer treatments. The fear of experiencing any one of them is common among people in the early days of a new diagnosis.
These conditions can often alter a patient’s self-image and how they identify in the world around them. Some may want to isolate further from their family and friends, but what’s important to keep in mind, Joyce says, is that “there is loss and a change in your body, but you’re still you.”
When working with patients, Joyce suggests allowing time for the grieving process around physical changes to unfold naturally. This can sometimes be a slow period of adjustment – and it all depends on the patient and the changes they are facing.
Once a rapport is established between the patient and their healthcare worker, Joyce suggests offering advice on how they can reframe the situation in a more positive manner.
“I like to ask them, ‘What are your strengths? What have you done in the past that you’ve overcome?’ We encourage them to be creative and open.”
Introducing this type of mindful thinking can gently shift a patient’s outlook away from the negative mental chatter that can often consume them in the early stages of their treatment.
”I think teaching others to be mindful in the moment, and not looking ahead continuously can really help,” adds Joyce.
It’s also important to remember that a patient’s life is not over just because of a physical change to their body. Some side effects may only be temporary – and many times patients are able to resume old hobbies and interests that bring them joy.
Joyce recently encountered a patient who had to undergo an above-the-knee leg amputation. During his grieving process, the man couldn’t fathom how he would ever be able to ride on his beloved Harley Davidson without two full legs. Eventually, the patient was able to overcome his fear and now embraces his new prosthetic.
“The more knowledge we were able to provide him about the loss of the limb, the more empowered he became to make decisions about moving forward, rather than saying, “I’m done, I can’t do this,’” she says.
By returning to normal, everyday life, patients can reconnect to their community, and be reminded that life is made up of many different things – not just their diagnosis.

Coping with the Emotional Changes, Too
Loving one’s body is not always something patients are thinking about – especially when coping with a new diagnosis or adapting to a new treatment plan. Some feel betrayed by their bodies and what’s happening inside of them, while others might remain in complete denial.
These emotional challenges and roadblocks are common, says Joyce. “When someone hears that they are diagnosed with cancer, they’re in shock,” she says. “They’re not thinking about the self-image. They’re thinking about death.”
To help a patient move towards emotional acceptance of their new self-image, Joyce suggests meeting them where they are. This may require giving the patient additional space to grieve and to speak honestly about their emotions. In other words, jumping directly into “self-love” pep talks and positivity speeches might not be the best strategy.
“Grief is very important, and we don’t want to minimize that,” she says. “The best thing that a patient can do to improve their quality of life is to be open about their cancer.”
If a patient or loved one isn’t good with communicating their feelings, consider the implementation of regular family meetings. These conversations can happen as frequently as once per week, and Crossroads team members can be in attendance to help navigate sensitive topic matters. They can also offer knowledge from their own learned experiences.
Most importantly, no topic should be off limits. So if a patient’s family or loved ones cannot provide the basic support needed, Crossroads social workers can connect their patients to support groups and bereavement coordinators who specialize in grief and loss.

Thinking Outside the Box with Treatment Options
How a patient copes with their cancer diagnosis and treatment plan will ultimately be up to them. But the practices of being mindful or sitting for meditation are two tools that are now being used more frequently to help patients calm their anxieties around their diagnosis.
These simple acts of being present and in the moment can not only improve the patient’s emotional state of mind but also, in some cases, improve their overall health, says Joyce.
“You’re forgetting about tomorrow and how ‘I’m not going to be able to get in the car and drive,’” she says, referencing the mental chatter that can become all encompassing. “So when you’re being mindful of just that moment, you can feel your body healing.”
Another exercise to add to a patient’s treatment is art therapy. Drawing, working with clay or painting are a few activities that Joyce recommends that can help soothe anxieties and almost anyone can do.
This type of creative play with various materials can help someone who is stuck become unstuck. For some patients, it may be easier to express a difficult feeling or experience.
Making something by hand is also a great activity for children to do with their parents. Not only will they spend some quality time with their loved one, but they’ll also have a special memento from this difficult time, says Joyce. Some of her patients have held onto these memories for decades.
“Art can be so powerful,” she says. “It’s a takeaway because it’s something they’ve created together.”
For more information about how Crossroads does more for patients, visit our website of give us a call at 1-888-564-3405.
If you found this information helpful, please share it with your network and community.
Copyright © 2020 Crossroads Hospice & Palliative Care. All rights reserved.




