Starting Strong: Healthcare Trends for 2022

As the world marks two years since the COVID-19 outbreak, many may be looking to 2022 with apprehension. The pandemic has changed the way we do almost everything — and that’s especially true for healthcare providers. Unsurprisingly, 2022 may look very similar to 2021 in the palliative and hospice care industry as the pandemic continues.
“Unless this virus stops mutating, 2022 will mainly be a repeat of 2021,” said DeAnna Looper, Chief Compliance Officer at Crossroads Hospice & Palliative Care. “Losses in staff and decreased access to long-term care will unfortunately persist.”
But as we look forward to the upcoming year, we do so armed with the lessons of the past two years, as well as facing the same challenges.
“As a sector, we’ve also identified tactics that are working well,” said DeAnna, “and we can expect those successes to continue, too.”
Here are a few trends – some new and some existing – that we can expect in the coming year.

Continuing Virtual Care
The COVID-19 pandemic has had a significant impact on healthcare delivery across the globe. Born out of necessity, virtual health has a growing role in primary care, managing chronic conditions, and increasing access to mental health treatment. This is particularly true in the senior care industry. The adoption of digital health was particularly well-suited to today’s seniors, who are more tech savvy than ever.
Using video calls and telehealth appointments have become commonplace, a trend that is likely to continue in 2022 to streamline palliative and hospice care.
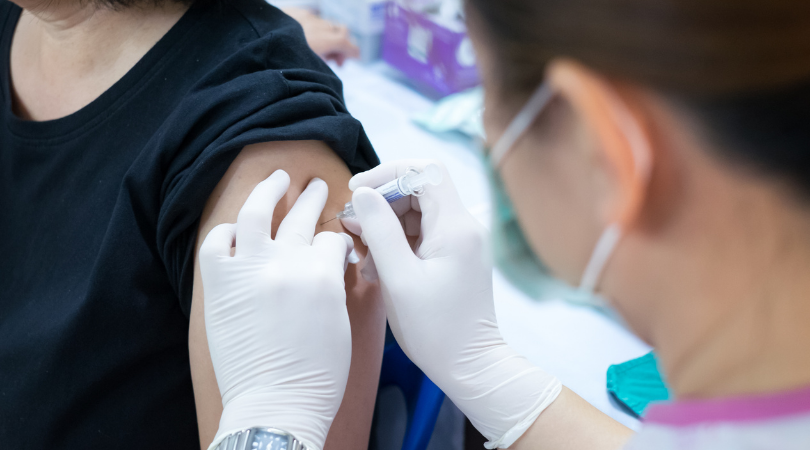
Mandating Vaccines
One major difference between this year and next is the widespread availability of vaccines. They slowly became more available in 2021 and, looking ahead to 2022, they continue to be our first line of defense against the spread of COVID. But, as vaccine mandates become more prevalent, that may impact long-term care.
“Mandating a vaccine will cause issues within some agencies due to the inability to enter the facilities and provide services,” said DeAnna. “At Crossroads, we have made vaccinations mandatory for working in and visiting our facilities. Those few who have been granted an exemption under Title VII will be unable to work as normal from those vaccine-mandated facilities, impeding their ability to provide the same services.”
In addition to the effects on staff, vaccine mandates affect friends and family who wish to visit a patient in palliative or hospice care.
“Over the past two years, we’ve seen families not able to visit their loved ones in facilities due to the restrictions,” said DeAnna. “As a result, many patients died without having contact with family–which is something that we never want.”

Suffering Staff Losses
At the onset of the COVID-19 pandemic, the healthcare profession saw a steep drop in employment. The majority of those jobs did come back, but the sector is still operating at nearly a 3% deficit.
“The loss in staff is due to a multitude of reasons, meaning there is no easy fix,” said DeAnna. “Some have had to return to their families as primary caregivers due to the closing of daycare or spouses losing their jobs. COVID also gave people – not just healthcare workers – new perspectives on what they want, and want they don’t want. Many have personal reasons to leave healthcare.”
Although the sector is building back up, we will continue to see losses among palliative and hospice care workers.

Treating the Whole Person
Hosopice and palliative care providers may face an increase in patients seeking end-of-life care. The COVID-19 pandemic exacerbated existing systemic issues for traditionally vulnerable populations. A recent study shows that several shelter-in-place mandates had a tendency to delay routine doctor visits and preventive screenings, leading to an increase in late-stage diagnoses and advanced medical issues.
The same is true for caregivers, who are facing similar challenges–but they are compounded by the tendency for caregivers to neglect their own health. Social isolation and uncertainty also gave rise to mental health and substance abuse.
Health, wellness, and emotional well-being must be looked at holistically as we move into 2022 and treat the side effects of the pandemic. For hospice and palliative care providers, this means being prepared for terminal illnesses to have gone undetected–and to provide support for families, friends, and self-appointed caregivers.
The past two years have been challenging, but if we look closely enough, those challenges have led to advancements in care. As the world continues to struggle with a global pandemic and its effects, we begin 2022 stronger, wiser, and more prepared than ever.
To learn more about our services, please call 1-888-564-3405.
If you found this information helpful, please share it with your network and community.
Copyright © 2021 Crossroads Hospice. All rights reserved.




